How can we build resilience facing a chronic illness?
Lilla Nafradi, Ph.D.
Resilience is a complex concept that, when interpreted as a personal disposition, refers to the individual’s ability to successfully adapt to adversity. Resilience is defined as one’s capacity to bounce back and recover from challenging events or to sustain functional capacity and participate in personally and socially meaningful activities despite the detrimental life situations and, in some cases, it might encompass post-traumatic growth. Resilience can be discussed in diverse contexts, one example being a chronic illness. The scope of this article is to tell Darren’s story—who now had to cope with having a chronic condition for more than two decades—and share his personal experience of developing resilience.
Darren Cawley (41) is a loving husband, a happy father of two, a respected motivational speaker and an accomplished sportsman from Ireland. He is also the recipient of two kidney transplants.
Darren’s patient journey started at the age of 20, when he was an ambitious, fit and healthy student, pursuing a degree in sports at the University of Bedfordshire, UK. He went for a check-up due to having problems with his eyesight. His unexpected diagnosis was kidney failure.
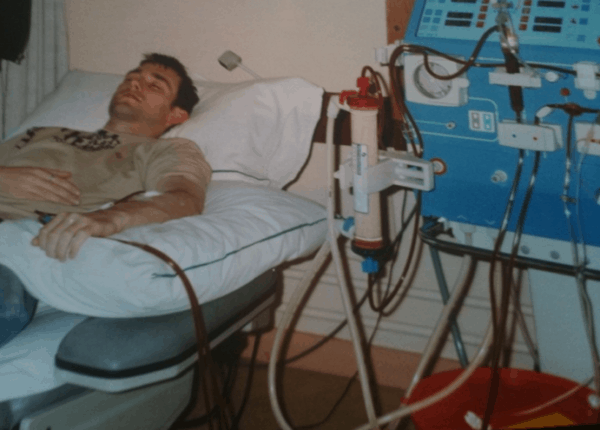
Consequently, he needed to adjust during the course of weeks to a very different life, in which hospital visits, dialysis sessions, blood pressure monitors, IV lines, diet and fluid allowance became his new everyday reality. He got his first transplant when he was only 22 years old.
Less than 2 years later, due to an infection, Darren was informed that his transplanted kidney was not working and he would need a transplant nephrectomy.
“This to me meant all the pain and suffering of a transplant, without the happy ending. With this news I was also told I would spend several years on dialysis before I could even attempt another transplant. Therefore, my foreseeable future was ill health and dialysis sessions in hospital every two days. I was 24 years old at the time,” says Darren. Nine years later, in 2011, he finally got his second kidney transplant. By that time, at the age of 33, he had more than 1,700 hospital sessions.
Here he reflects on how he became an exemplar of a resilient person, in its purest form, by turning kidney failure into a catalyst for change and personal growth, under the conditions that life and ill health has laid out for him.
“Resilience to me is having the mental capacity to live life to the fullest despite of the setbacks and adversities. In a sense, it is a sort of mental gymnastics developed over time. A skill that allows me to bend during difficult and challenging times, but not break,” Darren explains.
Acceptance is a first step in moving forward
“Acceptance doesn’t mean resignation; it means understanding that something is what it is and that there’s got to be a way through it”. – Michael J. Fox
Acceptance has been shown to be an adaptive reaction to unchangeable situations, such as living with a chronic condition. Those patients who actively accept their illness can incorporate the disease into their daily routine, yet they do not let their lives to be completely disrupted by the treatment.
“Personal acceptance of my situation was a big step forward and this took time. I was glad it took time, as it was an enormous lesson to learn. I now believe that when you accept your adversity and the personal responsibility of having to deal with it, you can begin to move forward. Paul Coelho described it perfectly in his book, The Alchemist: “And, when you can’t go back, you have to worry only about the best way of moving forward.” Moving forward became my goal. Role models, reading, exercise, affirmations and a positive mindset were my teachers.
One particular role model was a transplant athlete from Ireland. One of the main reasons I looked up to him was because he was able to run a big family business. He also got married and had a child before I did. To see a fellow patient living such a normal and successful life, with renal failure, was very motivating for me. If he could do these things, then so could I!
This lesson, relatively early in my health issues and hard learned, has stayed with me. It has given great confidence and solace when other difficult situations in life came my way.”
Communication: The key to finding the right way to support a loved one
Family and friends are an integral part of recovery and coping with health issues. However, having well-meaning intentions is not a guarantee of really helping someone. Only by listening to patients can we provide the right form of support, at the right time.
“It is a challenge for both the patient and the supporting group. Patients want the autonomy to live as normal a life as possible; however, this is challenging within the confines and limitations of an illness. It certainly takes time to process “bad news” and while well intended, friends and family flock to help you and find solutions, the patient is often not ready to move so fast. This can be difficult to communicate.
Support and help are two very different words. Family and friends often need to understand that a patient does not always want or need help. Help can feel intrusive when people push their thoughts and opinions, often unasked for, at the patient. Support is much more useful. The patient may struggle to uncover the realities of living with an illness and this often needs to happen on their own. When having an illness is processed internally, the support and help of the family and friends then becomes essential.
Overall, patients need help and support from those closest to them, there is no question about this. However, until the patient decides what course this may take, conflict often occurs. The communication skills necessary for these types of conversations are not always there, so it leads to frustration for the patient and creates a sense of uselessness and impotence for those striving to support. I see communication as the key to find solutions between the need of families to be involved and how much involvement the patient desires from those offering.”
The role of health care professionals: Interacting with “the person behind the patient”
A relationship with health care professionals that follows the precepts of the patient-centered care can become a significant resource for the patient that can lead to an increased sense of resiliency.
“If you trust your healthcare team and the medicine, it greatly helps in having successful outcomes. Nurses over the years have greatly enhanced my coping skills by simply translating the scientific medi-speak to the ordinary language in that the patient can understand and process health information and, equally importantly, listening to the cares and concerns I have had. Nurses understand and deal with the person behind the patient and I have been lucky to call many nurses my friends and look to them with gratitude, thanks to hundreds of kindnesses over the years.”
A refined self-concept: “A healthy person with certain health issues”
Maintaining socially and personally meaningful activities, being physically active and meeting with people who can be role models for us can positively influence our self-esteem, which, in turn, can promote adaptive disease management behaviors, self-care and well-being.
Sport has always been a source of strength for Darren and an opportunity to meet people with the same health condition, who helped him to recognize his own potential and develop a growth mindset.
After recovering from his first transplant, he won two bronze medals at the World Transplant Games (2001) in Japan and a gold medal at the European Transplant and Dialysis Games (2002), as a member of the Irish national team.
“For me the Transplant & Dialysis Games were a revelation—not just for the numerous benefits of exercise—but the introduction of role models to my life. It was the first time I encountered people with the same health issue as me but with a different, more positive attitude. I came to realize that I had a specific health issue, kidney failure, and that my head, legs, arms, heart and lungs, etc. were all working perfectly. Well, that they had the potential to work perfectly. Before this, I viewed myself as being “sick”, as in, a sick person. After the Games, I came to realize I had the potential to be much more than a sick person, but a healthy person with certain health issues. This created a kind of paradigm shift within me.”
Sport remained an important part of Darren’s life. In fact, he has decided to compete once again this year at the European Transplant & Dialysis Games in Dublin.
“I am really looking forward to participating in the Games, but it will be tough to get back into the fitness levels I will need to compete!”
Living the best life you can with renal failure
A major building block of resilience is the capacity of not only accepting having to live with a chronic condition, but also trying to make the best of the situation.
“Who would I have become if I did not get kidney failure? As I have kidney failure over 20 years now, it is impossible to say. Before that, I would say, I was a young man who had yet not found himself. I was pretty quiet and uncertain about my future. Now I am an international speaker, a future undreamed and unconsidered before my health issue. Other positives of kidney failure have been representing Ireland at international sport events, and winning gold medals. I was good at sport before kidney failure, but I would never have been at a level to represent my country. Most importantly, on a personal level, I am married with two healthy and happy children; I guess life does not get much better in many ways.
Certainly such a disease affected my personality development and my life, and it has been challenging with many ups and downs, but I spend very little time dwelling on maybes and ifs”.
A true calling: “Sharing is caring”
Some people, who went through adverse life situations, are highly motivated to help others in need. Darren is definitely one of these people, becoming an international motivational speaker, who is sharing his journey with kidney failure to provide a unique source of inspiration to his audience. He was invited to deliver speeches at the European Parliament and several significant medical conferences and was voted the Highest Rated Guest Speaker at the EDTNA/ERCA conferences in two consecutive years (2014 and 2015).
“I try, in my own way, through speaking to help make struggles acceptable and overcome them the norm. I feel the best way to do this is where the message and the messenger are one. I aim to set a good example by being an example of a healthy patient, but who also “wears my blemishes openly.”
For me the skills, attitudes and characteristics I picked up outside the hospital are as important as the lifesaving treatment that I received inside the hospital. These include the importance of role models, the benefits of exercise, developing and maintaining a positive attitude, the use of affirmations, the importance of reading and continuous education and many more.
I think it’s important to say that we can only deal with our reality as it currently exists. For example, I have a transplant and I know that someday it will fail. For as long as it lasts, I will live this life. When it fails, I know I will have to live a different reality. I am confident that with the mental reserves built up in relation to resilience, self-confidence and attitude, I can survive and continue to be the best version of me I can be, no matter where my life leads.
With this in mind, I relish the challenge to serve as a role model in transforming thinking and to impact patient behavior in a positive way. I believe we can all find growth in adversity.”

About the Author:
Lilla Nafradi, Ph.D. is a Healthcare Communications Specialist, Psychologist and the author of several peer-reviewed scientific publications.
References
Compas, B.E. (2006). Psychobiological processes of stress and coping. Annals of the New York Academy of Sciences, 1094(1): 226-234.
Juth, V., Smyth, J.M., & Santuzzi, A.M. (2008). How do you feel? Self-esteem predicts affect, stress, social interaction, and symptom severity during daily life in patients with chronic illness. Journal of Health Psychology, 13(7):884–894. doi:10.1177/1359105308095062
Kralik, D., van Loon, A., & Visentin, K. (2006). Resilience in the chronic illness experience. Educational Action Research, 14(2): 187–201. https://doi.org/10.1080/09650790600718035
Luthar, S.S., Cicchetti, D., & Becker, B. (2000). The construct of resilience: a critical evaluation and guidelines for future work. Child Development, 71:543-562.
Náfrádi, L., Kostova, Z., Nakamoto, K., & Schulz, P. J. (2017). The doctor-patient relationship and patient resilience in chronic pain: A qualitative approach to patients’ perspectives. Chronic Illness, 14(4):256-70. doi: 10.1177/1742395317739961. Epub 2017 Nov 2.
Stewart, D.E., & Yuen, T. (2011). A systematic review of resilience in the physically ill. Psychosomatics, 52(3): 199–209.
Nakamura, Y. M., & Orth, U. (2005). Acceptance as a Coping reaction: adaptive or Not? Swiss Journal of Psychology, 64(4): 281-292.
Sodergren, S. C., & Hyland, M. E. (2000). What are the positive consequences of illness? Psychology and Health, 15, 85-97.
Zautra, A.J. (2009). Resilience: One Part Recovery, Two Parts Sustainability. Journal of Personality, 77: 1935-1943. doi:10.1111/j.1467-6494.2009.00605.x




